
POSTER ABSTRACTS
Materials should NOT be shared with those that are not registered for the conference. Poster abstracts are not proofed for spelling and/or grammar errors.
The poster and/or other information contained on this website may NOT be downloaded and/or used without prior written permission from all authors on the project. If you would like to be connected with the author(s), please email [email protected].
Cardiorespiratory coupling response to chest wall strapping in chronic obstructive pulmonary disease patients
Maggie Peng1, Iliya P. Amaza, MD2, Michael Eberlein, MD, PhD3, Melissa L. Bates, PhD4
1Scarsdale High School, Scarsdale, NY
2Department of Internal Medicine, University of Wisconsin, Madison, WI
3Department of Internal Medicine, University of Iowa, Iowa City, IA
4Department of Health and Human Physiology, University of Iowa, Iowa City, IA
Abstract
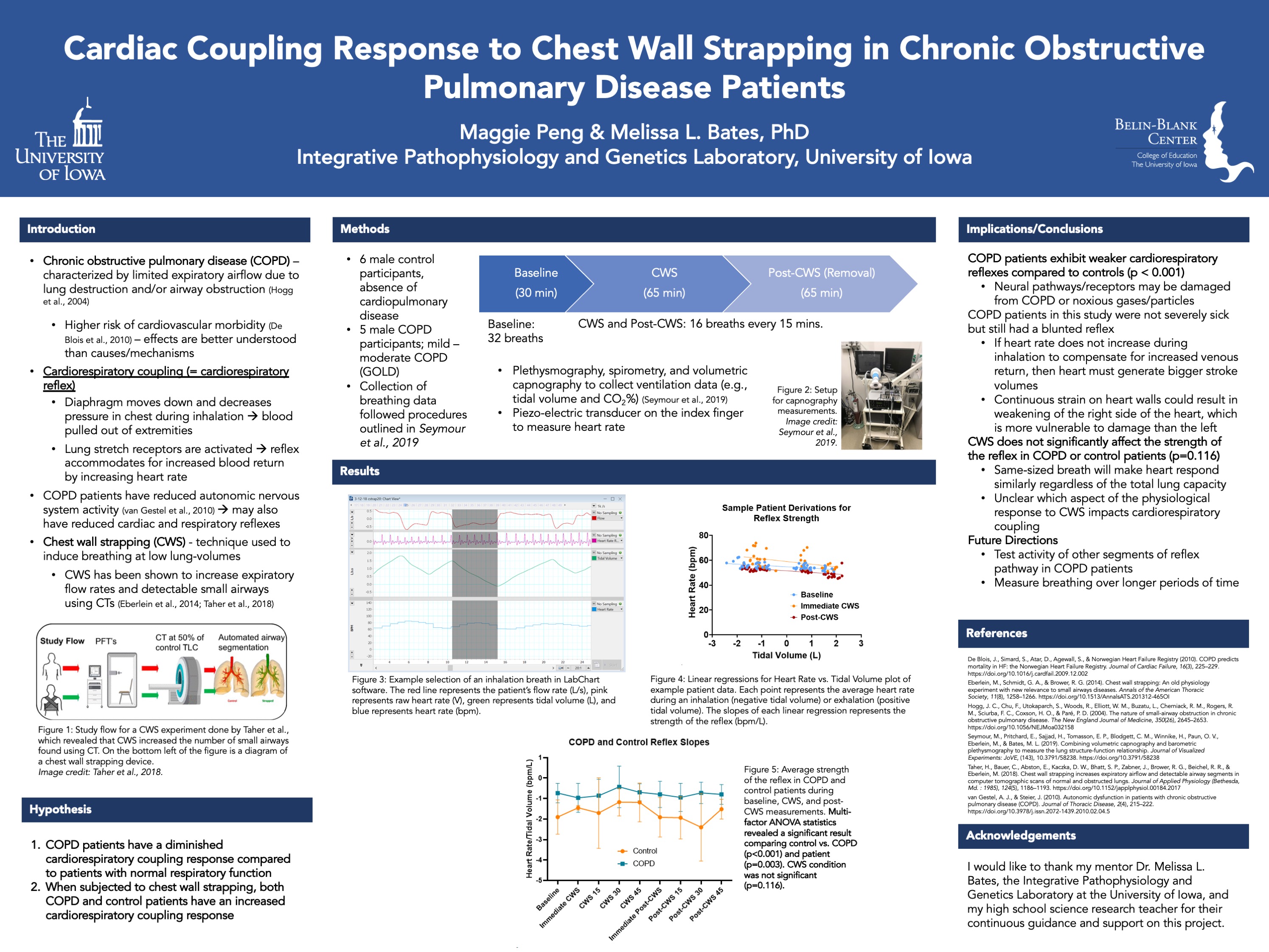
Chronic obstructive pulmonary disease (COPD) is characterized by limited expiratory airflow due to lung destruction or airway obstruction. Chest wall strapping (CWS) is a potential therapy technique that restricts the upper abdomen and induces breathing at lower lung volumes. CWS opens small airways in normal and obstructed lungs. Although the respiratory impacts of CWS have been examined, the relationship between CWS and the cardiovascular system, which is closely tied to ventilation, has not been well-established. Additionally, COPD patients have reduced autonomic nervous system activity, which may be reflected in cardiorespiratory coupling. Cardiorespiratory coupling increases heart rate during inhalation to accommodate for increased venous return. The strength of this relationship was evaluated during CWS in five male COPD and six male control patients by analyzing heart rate changes during ventilation cycles. Heart rate and ventilatory data were collected during baseline, CWS, and post-CWS removal periods. Average heart rate during each inhalation and exhalation was plotted against tidal volume, with the slope of the linear regression representing the strength of the cardiorespiratory coupling relationship (bpm/L). Multi-factor ANOVA statistics showed a significantly diminished strength in COPD patients compared to control (p<.001). There was no significant change in either group post-CWS, suggesting that the same-sized breaths will cause the heart to respond similarly regardless of the total lung capacity. A potential consequence of blunted cardiorespiratory coupling in COPD patients is strain on the right side of the heart, which must then pump larger stroke volumes. Blunted cardiorespiratory coupling is not further impaired by CWS.
Access PDF version to expand view.
